Exploring The Fundamentals of Medical Billing
A Guide for Healthcare Professionals
The healthcare industry is one of the most complicated systems in the world, with regular changes and updates. Managing patient care, scheduling, billing, insurance claims, healthcare compliance, and financial transactions can become overwhelming as time goes on. This is where medical billing services come in. Medical billing services simplify the process of billing and payment, ensuring that healthcare providers can focus on what they do best, taking care of their patients.
What is Medical Billing?
Medical billing is the process of submitting and following up on claims with health insurance or other companies in order to receive payment for services rendered by healthcare providers. It involves translating medical procedures, diagnoses, and treatments into standardized medical billing codes, which are then used to create invoices or claims for insurance reimbursement.
The process includes verifying patient insurance, ensuring accurate coding, submitting claims, and managing any denials or rejections. Effective medical billing ensures that healthcare providers are compensated for their services in a timely manner while complying with regulatory standards. It also helps in avoiding errors that could lead to claim denials or delays.
How Medical Billing Works
Medical billing works by translating healthcare services into standardized codes, submitting claims to insurance companies or patients, and ensuring proper reimbursement for services provided. The medical billing process broken down into three stages:
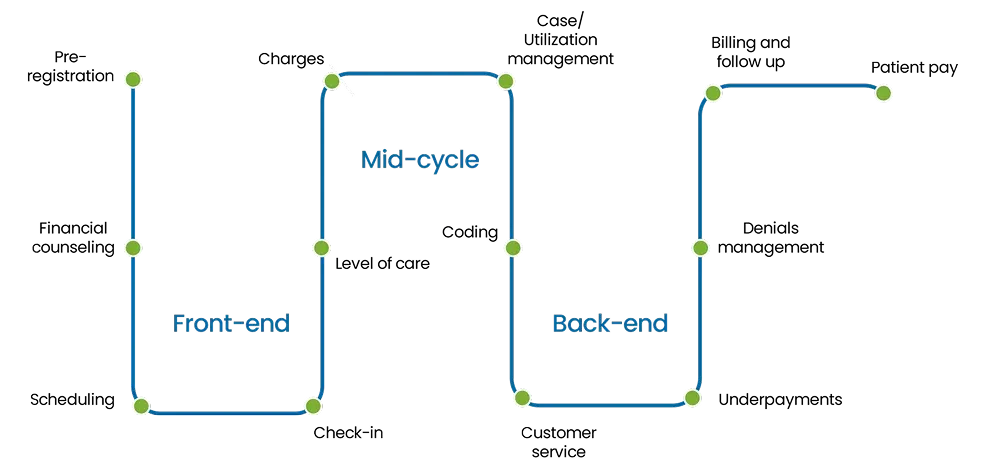
Front-End: This stage focuses on the activities before the patient receives medical services like patient scheduling, registration, insurance verification, and prior-authorization request.
Mid-Cycle: This stage involves activities during the period of patient care focused on accurate clinical documentation, charge capture, medical coding, and billing.
Back-End: This stage takes place after the patient received the healthcare service and biller focuses on processing claim, payment posting, resolved denial issues, and work on patient collection.
Types of Medical Billing Systems
There are three main types of medical billing systems that facilitate both healthcare professionals and patients with distinct characteristics within various health care practices.
Closed Medical Billing Systems: A closed medical billing system refers to a billing model suited for specific facilities or practices. Where an in-house healthcare billing department manages all aspects of the billing process and are not shared among different facilities, specialists, or others.
Open Medical Billing Systems: An open medical billing system incorporates external entities like insurance companies, third-party administrators, stakeholders, outsourced billing teams, and clearinghouses in the billing process. This model is typically used in larger healthcare organizations, where claims must be processed efficiently, often in real time, due to the interconnected nature of multiple specialties and departments.
Isolated Medical Billing Systems: An isolated billing system is a standalone billing process that functions independently from other healthcare management software, specifically tailored for patient care. This system is often used by smaller practices or independent healthcare providers who do not require traditional medical billing systems.
Types of Medical Codes Used in Billing Process
Medical billing used three main types of standardized codes to ensure accurate billing and reimbursement from insurance providers. Which are as follow:
1. CPT Codes (Current Procedural Terminology)
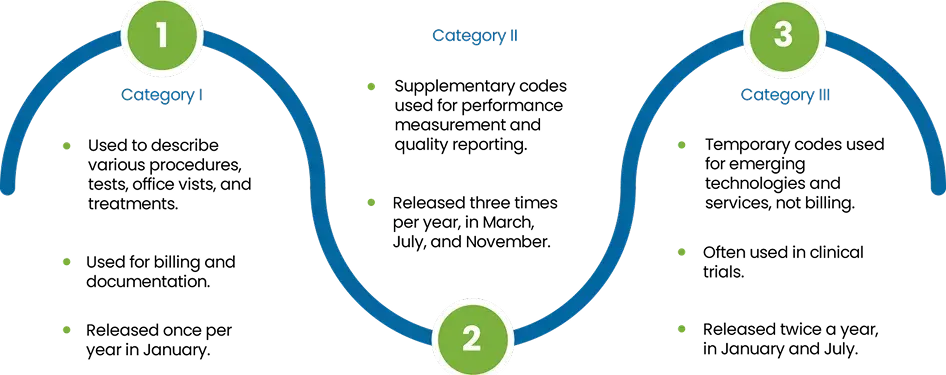
CPT codes are a standardized set of codes used by healthcare providers and payers to document and report medical services, routine check-ups, surgical procedures, and diagnostic tests. These codes help to render healthcare services provided during a patient visit, making it easier for the insurer to understand the treatment process thoroughly and determine the reimbursement ratio depending on it.
Example: A routine office visit might be coded with a specific CPT code like 99213, which corresponds to an evaluation and management service for an established patient.
2. ICD Codes (International Classification of Diseases)
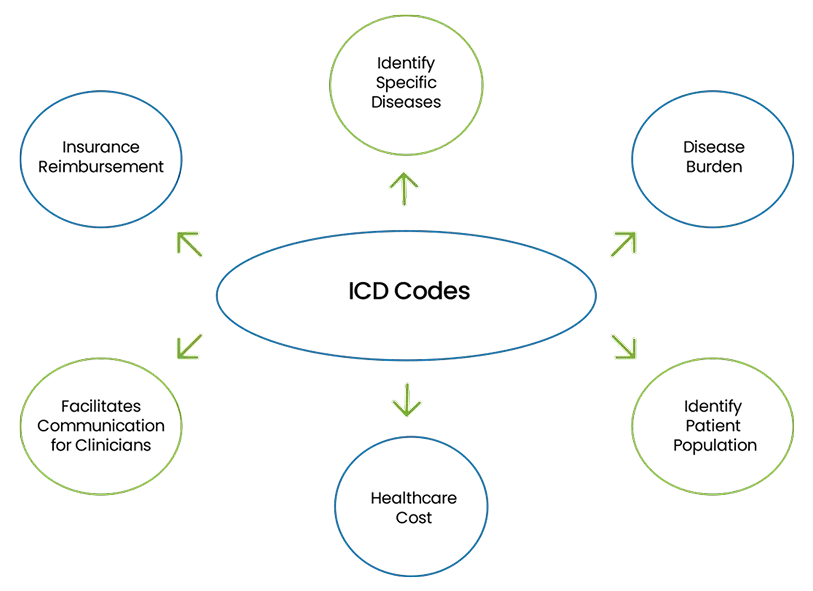
ICD codes are used to classify and code diseases, conditions, and other health-related problems. These codes help identify the reason for a patient’s visit, guiding both medical professionals and insurance companies in understanding the health issue being treated. Additionally, it ensures that the healthcare provider’s diagnosis is properly linked to the services provided, enabling proper reimbursement.
Example: If a patient visits for a knee injury to the lower leg, the ICD code may be range S80-S89, which refers to osteoarthritis of the right knee.
3: HCPCS Codes (Healthcare Common Procedure Coding System)
HCPCS codes are a set of codes used primarily for medical services and supplies not covered under the CPT code system, such as durable medical equipment (like wheelchairs, crutches, prosthetics), ambulance services, and certain drugs and medical surgical supplies. DME billing services help ensure that these items and services are billed accurately and reimbursed appropriately, minimizing the risk of claims denials.
Example: A HCPCS code like E0114 is used for crutches, underarm, wood, adjustable height.
Types of HCPCS Drug Codes-Primary
Type
Description
Issued By
Used For
J Codes
Permanent code for drugs dillable under Medicare
CMS
Community and hospital billing for outpatient physician administered drugs
C-Codes
Paid under the Hospital Outpatient Prospective Payment System (OPPS)
BCBS Associations and listed in HCPCS coding set by CMS
Non-Medicare Community and hospital billing for drugs and services
Q-Codes
Temporary codes for drugs billable under Medicare
CMS
Community and hospital billing for outpatient physician administered drugs
S-Codes
Temporary codes for drugs billable under Medicare
CMS
Community and hospital billing for outpatient physician administered drugs
Understanding Medical Billing Codes
HCPCS codes are a set of codes used primarily for medical services and supplies not covered under These medical codes ensure that the healthcare provider is reimbursed correctly by the insurance company. Accurate coding helps prevent claim denials, reduces administrative errors, and ensures a smoother payment process for both the provider and the patient. Incorrect or incomplete coding can delay payments and lead to financial discrepancies, making it vital to have trained medical coders and billers who understand the complex coding systems. Here are some coding certifications that are often mandatory based on regulatory requirements HCPCS codes help ensure that these items and services are reimbursed appropriately.
Entry-level Medical Billing and Coding Certifications
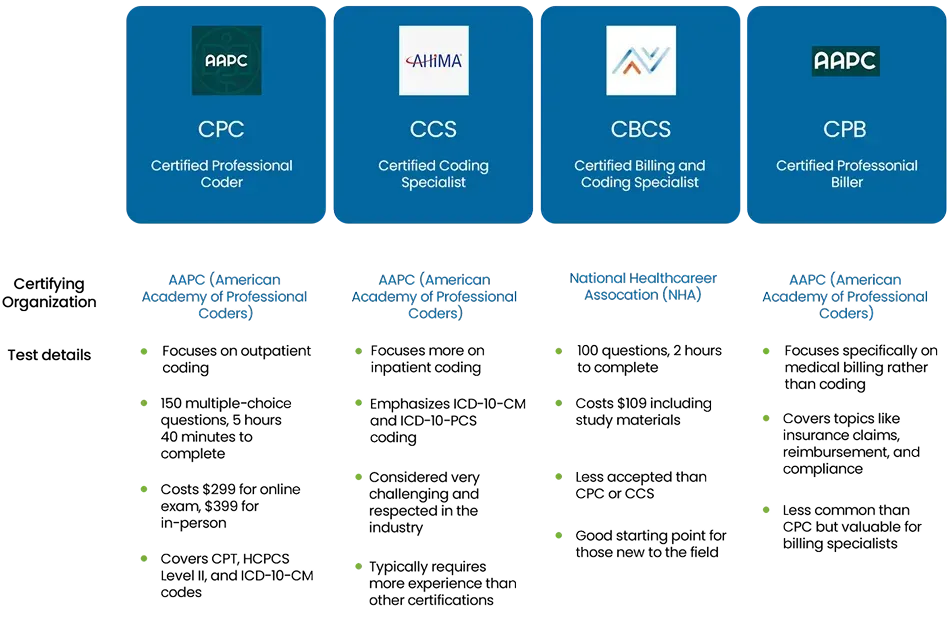
Step-By-Step Process for Medical billing
The process for medical billing involves coding services, submitting claims, and ensuring timely reimbursement through accurate patient documentation and compliance with regulations. The details for each step are as follows:
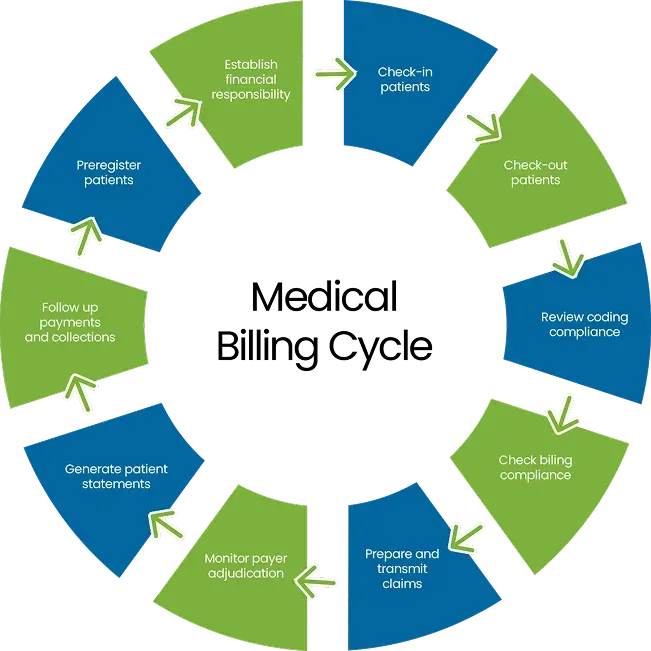
Step 1: Patient Registration
The initial and important step in the medical billing process is patient registration, where essential information is collected, like:
Patient details (Name, Address, DOB, Emergency Contact Detail).
Insurance detail (Primary, Secondary, Tricare).
Previous medical history.
Current reason for visit.
Step 2: Insurance Verification
Once the information is gathered, the very next step in the medical billing is to verify the patient insurance eligibility for specific medical services being provided. This include:
Verify active insurance coverage and policy details.
Ensure that required pre-authorizations are in place before services are provided.
Checking policies related to deductible, co-pays, and covered services.
Confirm if the provider is within the patient's insurance network.
Resolve any issues or discrepancies in coverage or information.
Step 3: Coding the Services
After patient registration and insurance confirmation, the next step is coding the services that were provided during the patient visit. This involves translating medical diagnoses, treatments, procedures, and equipment into standardized alphanumeric codes (ICD, CPT, and HCPCS). This step involved:
Describe medical services provided, prevention, special consultation, rehabilitation, mental health, and surgical care.
Justify medical necessity for appropriate diagnosis to reduce any error risk.
Facilitate accurate billing, while ensuring provided services align with proper code.
Use of proper billing modifiers for additional details about a service provided or procedural performed.
Ensure that the codes align with the specific requirements of the patient's insurance provider.
FYI : Encounter Documentation Essentials
For accurate billing, make sure to document:
Chief Complaint
Diagnostic Test Results
Procedures Performed
Proper documentation is vital to ensure a smooth and clean claim process, as incorrect or incomplete patient information can result in claim denial or delays, while impacting healthcare provider’s cash flow.
Step 4: Claim Submission
Once the services are coded correctly, the medical billing moves on the claim generation and submission to the insurance company. These step involves creating an electronic or paper claim form that include:
Patient demographics
Insurance information
Diagnosis codes
Procedural codes
Charges for service rendered
Two type of claim submission method used are as follow:
Claim Submission Method
Description
Advantages
Disadvantages
Electronic Submission
Claims submitted through a clearing house between healthcare providers and insurers.
Faster processing, fewer errors, reduced paperwork.
Requires technology and system setup.
Paper Claims
Claims submitted via paper forms (e.g CMS-1500, UB-04).
Can be used if electronic submission is not available.
Slower processing, more prone to errors.
The accuracy of the claim submission is important. If claims are not submitted correctly or on time, it can delay the reimbursement process or result in claim denials. Electronic submission ensures that claims are received by the insurer faster and with fewer chances of error.
Step 5: Claim Adjudication
After a claim is submitted, it enters the adjudication phase, where the payer decides the amount of reimbursement ratio. Insurance payer evaluates the claim to determine:
Patient eligibility
Coverage for the services billed
Adherence to payer policies
Accuracy of coding and charges
The outcomes of the adjudication process may include:
Full approval and payment
Partial payment with an explanation
Claim denial with a reason provided
Step 6: Payment Posting and Reconciliation
Once the claim is approved by the insurance company, the payer sends payments, an Explanation of Benefits (EOB), or Electronic Remittance Advice (ERA) to the healthcare provider’s account. The balance that remains after the insurance payment (i.e. the patient’s deductible, co-payment, or coinsurance) is then billed to the patient. Additionally, if the insurance company underpays or the payment is less than expected, the billing department must inquire and resolve any discrepancies. This might involve contacting the insurer to request additional payment or appeal a decision.
Importance: Accurate payment posting is necessary to maintain a clear record of the practice’s revenue. If payments are not recorded properly, it can lead to confusion about the balance, delays in collections, or financial discrepancies. crutches, underarm, wood, adjustable height.
Step 7: Patient Billing
After insurance payments are posted, the next step is patient billing for the remaining balance. The healthcare provider sends a full-detailed statement or bill receipt to the patient for the remaining or outstanding balance after the insurance company has paid. This includes amounts like co-pays, coinsurance, deductibles, and services not covered by insurance. Moreover, keeping a transparent communication with patients regarding their financial responsibility is mandatory for good relationships. The process should involved:
Clear Breakdown: The patient’s bill should clearly outline what has been covered by insurance and what they owe. The statement should also include information about how the patient can pay, whether through online platforms, by phone, or by mail.
Collection Efforts: If the patient fails to pay their bill timely, the healthcare provider may need to send reminders or take additional steps, such as setting up payment plans or referring the account to a collection agency.
Step 8: Follow-Up and Reporting
After submitting the claim, it’s necessary to follow up with the insurance company to check the status of the claim and address any issues such as:
If the claim is denied, the reason must be identified (e.g., incorrect coding, lack of coverage) and corrected for resubmission.
Sometimes insurance companies request further documentation (medical records or additional forms) before processing the claim.
Regular follow-up on claims ensures that they are processed and paid efficiently. Failing to follow up can lead to unpaid claims and decreased cash flow.
The last step included in medical billing is to generate reports under the set KPIs for all the trends in claim denials or payments to maximize the overall financial health of the practice.
Why is Medical Billing Important?
Benefits
Importance
Accurate and Timely Payments
Medical billing services help healthcare practices of any size to receive accurate and timely payment for services rendered by submitting accurate and complete claims to insurance companies.
Eliminate Errors and Denials
Professional billing services eliminate the chances of claims being denied or delayed by accurate patient documentation and coding, which helps ensure the chances of first-time claim approvals.
Improves Cash Flow
By streamlining the billing process and reducing old AR, medical billing services help maintain a healthy cash flow for the providers.
Regulatory Adherence
Medical billing services ensure that all billing processes comply with healthcare laws and regulations, including HIPAA, CMS and insurance guidelines, while eliminating the risk of costly penalties.
Saves Time and Resources
Outsourcing billing services allows healthcare providers to focus more on quality patient care, while all front-end and back-end tasks are handled by expert medical billers.
Cost-Effective
Medical billing software is often more affordable than maintaining an in-house billing team, saving on overhead costs like salaries and other training expenditures.
Handles Complex Insurance Plans
Billing services are experienced in managing complicated insurance policies, making it easier for healthcare providers to work with various insurers and plans without confusion.
Reduces Administrative Burden
Outsourcing billing services reduces the workload on medical staff, allowing them to focus on other critical tasks rather than dealing with billing and insurance issues.
Improves Patient Satisfaction
With an accurate billing process, patients can receive clear and understandable invoices, improving their overall experience and reducing confusion or disputes over charges.
Laws and Compliance Must Follow in Medical Billing
Compliance and regulations are the most important part in medical billing to ensure healthcare providers adhere to all legal and industrial standards while submitting any claim. Moreover, staying up-to-date with these rules helps prevent costly errors, audits, costly-penalties, and other legal issues while ensuring a timely and accurate payment clearance process.
Regulation
Details
Applicable To
HIPAA (Health Insurance Portability and Accountability Act)
Ensures the patient data confidentiality, integrity, and security of patient personal information.
Healthcare providers, payers, clearinghouses.
CMS (Centers for Medicare & Medicaid Services)
Oversees compliance with billing policies and guidelines for Medicare and Medicaid.
Providers billing Medicare or Medicaid
Medicare & Medicaid Fraud, Waste, and Abuse (FWA)
Requires compliance with specific billing practices and identifies fraud and abuse.
Healthcare providers, insurance companies, government programs
False Claims Act (FCA)
Prevents fraudulent billing practices and submission of false claims to government programs (e.g., Medicare, Medicaid).
Healthcare providers, insurers, government contractors
Key Payers in Medical Billing
In medical billing, there are several key payers who are responsible for reimbursing healthcare providers for services rendered to patients. These payers play an important role in ensuring that healthcare providers are compensated for their services. The primary payers in the medical billing process include:
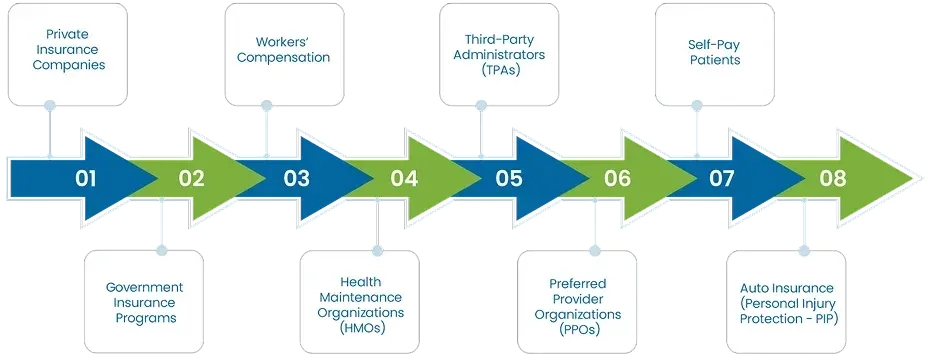
1. Private Insurance Companies
These are for-profit insurance companies that offer health insurance plans to individuals, families, or through employer-sponsored plans. Examples include companies like Blue Cross Blue Shield, Aetna, UnitedHealthcare, and Cigna. Private insurers receive claims from healthcare providers after services are rendered to insured patients. They review the claims based on the patient’s policy, benefits, and eligibility criteria’s and then provide reimbursement according to the terms of the insurance plan. Billing professionals need to understand the specific rules, coding, and reimbursement policies for each private insurer to avoid claim denials and delays.
2. Government Insurance Programs
Government programs represent a significant portion of healthcare coverage in the U.S. Healthcare providers submit claims to these government insurance programs when treating eligible patients. Only provide coverage for certain groups of people such as:
Medicare: Primarily for individuals aged 65 and older, or for younger individuals with disabilities.
Medicaid: Provides health coverage for low-income individuals and families, with eligibility varying by state.
CHIP (Children’s Health Insurance Program): Offers coverage to children in families who do not qualify for Medicaid but cannot afford private insurance.
FYI: Medicare, Medicaid, and CHIP have strict billing and documentation requirements, and the reimbursement rates for services are generally lower than those provided by private insurers.
3. Workers’ Compensation
Workers’ compensation is an insurance program that provides coverage for employees who are injured or become ill due to work-related activities. It covers medical expenses, rehabilitation, and lost wages. The billing process for workers’ compensation claims differs from other types of insurance, with specific codes and documentation requirements.
4. Health Maintenance Organizations (HMOs)
HMOs are a type of managed care plan that provides comprehensive health services to members through a network of doctors, hospitals, and other providers. Patients enrolled in an HMO plan typically need a referral from a primary care physician (PCP) to see a specialist. Healthcare providers must adhere to the HMO’s network requirements, and claims are typically submitted directly to the HMO for reimbursement.
5. Preferred Provider Organizations (PPOs)
PPOs are another type of managed care insurance plan that offers more flexibility than HMOs. Patients can see any healthcare provider, but they pay less when using providers within the PPO network. Healthcare providers who are part of the PPO network submit claims to the PPO, and the insurer reimburses them according to the patient’s plan. Claims can also be submitted for out-of-network care units, but the patient may have to pay higher costs.
6. Third-Party Administrators (TPAs)
TPAs are independent organizations that process claims for self-insured employers or insurance companies. They manage the administrative functions of insurance claims, such as claim processing and customer service, but do not assume the financial risk of the claims. Healthcare providers will submit claims to the TPA for processing, and they will reimburse the provider based on the employer’s health plan coverage.
7. Self-Pay Patients
Self-pay patients are individuals who pay for healthcare services from their own pocket money, without relying on insurance. This typically applies to those without insurance or those seeking services not covered by their insurance plans. Healthcare providers bill self-pay patients directly for services rendered. In some cases, providers may offer payment plans or discounts for patients paying in full at the time of service.
8. Auto Insurance (Personal Injury Protection - PIP)
Personal Injury Protection (PIP) is a part of automobile insurance that covers medical expenses for individuals involved in car accidents, regardless of who was at fault. If a patient is involved in an auto accident, healthcare providers submit claims to the auto insurer under the PIP coverage for treatment related to the accident. PIP insurance often covers medical bills, lost wages, and other expenses resulting from the injury.
Significance of Outsourcing Medical Billing in Healthcare Management
Outsourcing your medical billing services can help streamline the billing process, ensuring accurate claims and faster reimbursements. It helps healthcare providers focus on patient care while improving financial performance and maintaining compliance with regulations.
Revenue Cycle Management: Outsourcing medical billing services ensures efficient management of the revenue cycle, leading to timely payments, and minimizing delays and errors that could negatively affect a healthcare provider's cash flow and financial health.
Compliance Assurance: Outsourced billing companies always ensure their adherence to the latest regulatory standards, reducing the risk of legal consequences, audits, and costly penalties.
Patient Satisfaction: By outsourcing billing to experts, providers can ensure accurate and transparent billing, preventing misunderstandings and clearly outlining financial obligations, thus building trust and enhancing the patient experience.
Operational Efficiency: Overall reduces the administrative burden on healthcare staff, allowing them to focus on patient care rather than resolving billing issues or chasing down payments.
Error Reduction: Professional billing services minimize coding and documentation errors, reducing claim rejections and denials, and increasing the likelihood of prompt insurance reimbursements.
Financial Growth: Outsourcing billing functions can optimize reimbursement processes, boosting revenue and enabling healthcare providers to reinvest in their facilities, technology, and patient care services.
Challenges in Medical Billing Process
Some of the key challenges in medical billing process are as follow:
Incorrect coding or using outdated codes can result in claim denials or underpayments.
Patient insurance eligibility can be time-consuming, especially when patients change insurance plans or policies.
Claims can also be denied or rejected due to missing documentation or incorrect patient information.
Insurance companies may offer varying reimbursement rates for the same services depending on the policy and provider contracts.
Compliance with complex and strict regulations such as HIPAA, the Affordable Care Act (ACA), and Medicare/Medicaid policies can be difficult.
Patients may face difficulties understanding their bills, leading to confusion, complaints, or delays in payment.
Submitting claims to multiple insurers or dealing with third-party payers who may have different requirements and documentation standards.
Variations in billing practices and forms across different insurers and healthcare providers.
Many insurance companies have strict time frames within which claims must be submitted, and missing these deadlines can result in claim denials.
The risk of fraud, including improper billing for services not provided or upcoding (billing for a more expensive service than the one actually provided).
Difficulty in collecting payment from patients who either do not have insurance or have insufficient coverage.
Future of Medical Billing
The future of medical billing is in the significant transformation, driven by advancements in cloud-based technology, AI automation, telemedicine’s with evolving healthcare models. As healthcare continues to move toward value-based care models, revenue cycle management systems will need to adapt to ensure accurate reimbursement based on patient outcomes rather than just the volume of services provided.

AI and Automation: AI and automation are streamlining medical billing by handling repetitive tasks like data entry, claim tracking, and error detection. These automated integrated technologies reduce human errors, speed up claim processing, and improve overall efficiency in the billing workflow.
Cloud-based Medical Billing Solutions: Cloud-based medical billing systems like PMS (Patient Management System) allow healthcare providers to manage billing processes from anywhere, offering real-time updates and secure access to data. PMS solutions enhance collaboration, reduce IT costs, and ensure compliance with data security regulations.
Patient-Centric Medical Billing Solutions: Patient-centric billing solutions with integrated EHR/EMR features focus on clear communication, simplifying billing statements, and offering flexible payment plans. This approach helps improve patient satisfaction by making billing more transparent and manageable for patients.
Common Abbreviations Used in Medical Billing
Listed below are some of the common terms and abbreviations used in medical billing, and as follow in the guide as well:
Abbreviation
Full Form
DME
Durable Medical Equipment
BHP
Basic Health Program
NPI
National Provider Identifier
TIN
Tax Identification Number
EMR/EHR
Electronic Medical Records / Electronic Health Records
CPT
Current Procedural Terminology
HCPCS
Healthcare Common Procedure Coding Systems
ICD
International Classification of Disease
CLIA
Clinical Laboratory Improvement Amendments
POS
Place of Service
ROI
Release of Information
ASC
Ambulatory Surgery Center
AOB
Assignment of Benefits
EGHP
Employer Group Health Plan
ABN
Advance Beneficiary Notice
ATC
Applied to Deductible
RCM
Revenue Cycle Management
EOB
Explanation of Benefits
ERA
Electronic Remittance Advice
HIPAA
Health Insurance Portability and Accountability Act
CMS
Centers for Medicare and Medicaid Services
CHIP
Children's Health Insurance Program
HMO
Health Maintenance Organization
PPO
Preferred Provider Organization
EFT
Electronic Funds Transfer
PCP
Primary Care Physician
PHI
Protected Health Information
EIN
Employer Identification Number
ACA
Patient Protection / Affordable Care Act
FCA
False Claim Act
HCFAC
Healthcare Fraud and Abuse Control Program
TPL
Third-Party Liability
Streamline Your Revenue Cycle with Expert Medical Billing
Medical billing is a critical aspect of the healthcare industry that ensures providers are accurately and timely reimbursed for their services. The process involves patient registration, coding, claim submission, payment posting, and patient billing. By implementing best practices, staying compliant with regulations, and utilizing the right tools, healthcare providers can streamline their billing processes, minimize errors, and enhance their revenue cycle management.
Outsource your medical billing services with Quantum Health Services LLC. Trust us with your complex claim forms while you can focus on quality patient care. Contact us today to ensure the smooth processing of your claims.
Talk to a Billing Expert
By outsourcing your billing services to us, you can expect revenue growth of up to 20%
Get in Touch with us
We’re here to help anytime

Call Us

Mail Us

Opening Time
Mon -Sat: 7:00 - 17:00

Quantum Health Services is an independent medical billing and revenue cycle management company serving healthcare providers. We are not affiliated with Quantum Health healthcare navigation or insurance services. Our platform connects practices with trusted billing specialists and streamlined support solutions to help optimize revenue cycle performance and simplify medical billing operations.
©2026 | Quantum Health Services LLC | All rights reserved.



